
Periodontal disease is the more advanced version of gum disease. Gum disease affects the gums around your tooth where is periodontal disease affects of the bone supporting your tooth. If this becomes infected it can ultimately result in severe pain and tooth loss.
Gum disease progresses painlessly on the whole but can be detected early by a dentist. This article looks at 10 interesting questions about periodontal disease and how it develops from gum disease.
The best place to start talking about periodontal disease (periodontitis) is to take a brief look at gum disease (gingivitis). Gingivitis is characterised by:
If you have any one of the above characters you may have the early signs of gum disease.
Bad breath can also be a symptom but is not always present.
Not necessarily. Gum disease is a progressive disease going through different stages. At an early stage your gums may just be puffy and red only bleeding as the gum disease progresses. You may find that you’re able to keep the gum disease under control at home and indeed make some progress towards healing. If you do this you may find that the gums bleed less or not at all but the gum disease is still present as you have puffy or red gums.
If this is the case then the gum disease is not over and could easily advance again. You should monitor the situation and if the puffy or redness also disappears then you may have been successful in treating the gum disease yourself. If the puffy or redness remains then we recommend you visit a dental hygienist.
Because gum disease is caused by plaque and tartar around the outside of your teeth it’s important to ensure you clean your teeth well and remove this plaque. This can help to reduce inflammation of the gums and stop the plaque building up again.
Yes. You may find that professional cleaning is required to improve your oral health and remove any plaque which is built up around the gum line. However, if the gum disease is left untreated then it can progress onto the more serious periodontitis which can result in tooth loss.
We haven’t been able to find any research which correlates gum disease with early death. However there is research to indicate that the bacteria involved in gum disease are also present in a range of other potentially life threatening conditions, as well as affecting your immune system. Having gum disease does indeed give you a higher risk of developing some of these other conditions including:
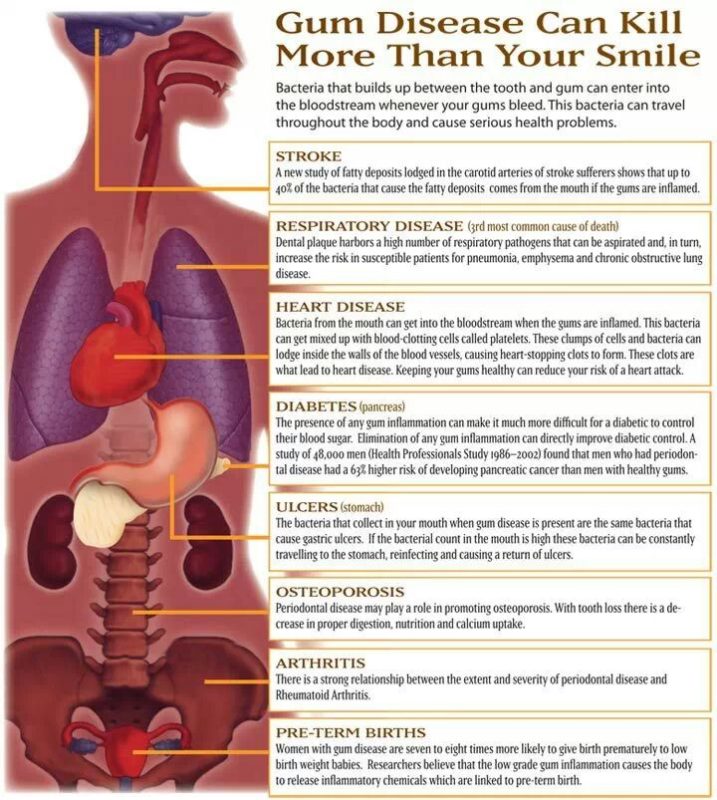
A new study of fatty deposits lodged in the carotid arteries of stroke sufferers shows that up to 40% of the bacteria that cause the fatty deposits come from the mouth if the gums are inflamed.
Dental plaque harbours a high number of respiratory pathogens that can be breathed in and leave you more susceptible to pneumonia, emphysema and chronic obstructive lung disease.
The bacteria in gum disease can get mixed into your blood, they specifically mix with the blood clotting cells which can lodge inside the walls of blood vessels causing heart attacks.
If you have other risk factors associated with the conditions above then maintaining good oral health and keeping gum disease at bay should be a high priority.
If you have periodontal disease then you have already gone through the gum disease. Gum disease alone has been linked to strokes, respiratory disease, heart disease, diabetes and ulcers. Periodontal disease is therefore linked to these other systemic health issues.
No. Interdental brushing in itself will not stop periodontitis or gum disease. However, interdental brushing IS an integral part of a good oral health care routine which should include:
If you follow this simple health care routine then you should avoid gum disease and a more serious periodontitis.
Because periodontal disease is progressive it means that once the periodontal disease has taken hold then you have already gone past the gum disease stage. It is only at the gum disease stage but you can treat it by yourself by modifying your oral health regime.
Yes. This is because periodontal disease is the second stage following on from gum disease. Periodontal disease can affect the root of your tooth, the periodontal ligament, the bone and the blood vessels around your tooth making it far more serious than gum disease.
You would have to floss quite hard in order to make this happen. If you floss too hard you may inflame the gums and introduce gingivitis. This can then be a quick link to periodontitis and periodontal pockets. The trick is to not floss too hard in the first place. When you visit your dental hygienist ask about flossing, you can then demonstrate what you do and your hygienist will be able to take you if this is too hard.
The exact mechanism of how periodontitis and diabetes are linked is not fully understood. There does however seem to be a two-way relationship. Susceptibility to periodontitis is increased by approximately 3 times in people with diabetes. Whilst the links are not fully understood they are thought to involve aspects of immune functioning, neutrophil activity, and cytokine biology.
There are also links to more severe ischaemic heart disease for diabetics who also have periodontitis meaning oral and periodontal health should be of prime importance to any one with diabetes.
There are essentially 4 periodontal surgery treatments:
A pocket is where the gum is not attached around the root of the tooth. This creates a large fold in the soft tissue which can become infected. Pocket reduction involves removing of any infected area and cleaning up any damaged bone, this allows the gum (soft tissue) to reattach in its normal way.
As periodontal disease progresses the bone and gum received giving the impression of the tooth looking very long, hence the phrase “long in the tooth”. This can be quite extreme with periodontitis so a gum graft will use soft tissue from another area of your mouth to graft over the area that has been lost.
If the disease has caused lots of bone loss then this can result in tooth loss eventually. Using bone regeneration techniques the bone can be restored to support your teeth better.
This is similar to the regular scale and polish you will receive at the dentist although this goes much deeper down the root.
Back to Blog“I cannot thank you enough for my experience, I phoned as a non registered patient in need of an emergency appointment and as a very…”
“Thank you Dapo and your dream team ❤🥰❤ I feel like I've been absolutely pampered with my recent treatments....and who would have ever thought that…”
“I just wanted to thank you again for how well you all treated my mum yesterday. She was very nervous but you were so kind…”
“Really great!!”
“I couldn’t stop looking at my teeth on the way home, you’ve done an amazing job - thank you so so much, you’re the BEST!!”


Teeth straightening is a minimally invasive and affordable treatment.
Learn more
• Step free access
• Wheelchair access
• Car parking
• Disabled parking


